CDC Warns of Cow-to-Human Transmission of H5N1 Bird Flu in Texas

By
The CDC has issued a health alert after cow-to-human transmission of H5N1 avian influenza in Texas, marking a worrying development in the spread of this highly pathogenic virus, which affects various species globally and presents potential pandemic risks.
A Texas farm worker contracted the H5N1 virus from dairy cattle, indicating a new transmission route for the virus.
” data-gt-translate-attributes=”({“attribute”:”data-cmtooltip”, “format”:”html”})” tabindex=”0″ role=”link”>viruswhich presents a high mortality rate and various symptoms in humans.
The US Centers for Disease Control and Prevention (CDC) has issued a health alert after the first case of H5N1 avian influenza, or bird flu, apparently transmitted from a cow to a human.
A Texas farmworker contracted the virus during an outbreak in dairy cattle. This is the second human case in the United States; a poultry worker tested positive in Colorado in 2022.
The virus strain identified in the Texas farmworker is not easily transmissible between humans and therefore does not pose a pandemic threat. But it is nevertheless a significant development.
A person has tested positive for bird flu after being exposed to cows suspected of being infected with the virus. This is the second time a human has been infected with H5N1 in the United States https://t.co/jJidEQbIEF
– Scientific American (@sciam) April 4, 2024
Some information about avian flu
There are two types of bird flu: highly pathogenic or low pathogenic, depending on the level of illness the strain causes in birds. H5N1 is a highly pathogenic avian flu.
H5N1 first appeared in 1997 in Hong Kong, then in China in 2003, spreading via wild bird migration and the poultry trade. It has caused periodic outbreaks on poultry farms, with occasional human cases.
Influenza A viruses such as H5N1 are divided into variants, called clades. The only variant causing the current epidemic is the H5N1 2.3.4.4b clade, which appeared in late 2020 and is now widespread globally, particularly in the Americas.
In the past, outbreaks could be controlled by culling infected birds, and H5N1 died out for a time. But this has become increasingly difficult due to the escalation of epidemics since 2021.
Wild animals are now in the game
Waterfowl (ducks, swans and geese) are the main global spreaders of avian influenza, as they migrate around the world via specific routes that bypass Australia. The main hub of waterfowl migration in the world is Qinghai Lake in China.
But there have been increasing numbers of infected birds other than waterfowl, such as true thrushes and raptors, which take different migration routes. Worryingly, the infection has also spread to Antarctica, meaning Australia is now under threat from different birds.
” data-gt-translate-attributes=”({“attribute”:”data-cmtooltip”, “format”:”html”})” tabindex=”0″ role=”link”>species who fly here.
The H5N1 virus has spread in an unprecedented way since 2021, and an increasing number of mammals, including sea lions, goats, red foxes, coyotes and even domestic dogs and cats, have been infected in the whole world.
Wild animals like red foxes that live in peri-urban areas provide a possible new route of spread to farms, pets and humans.
Dairy cows and goats have now been infected with H5N1 on at least 17 farms across seven US states.
What are the symptoms?
Globally, there have been 14 human cases of H5N1 clade 2.3.4.4b, and 889 total human H5N1 cases since 2003.
Previous human cases have presented with severe respiratory illness, but H5N1 2.3.4.4b also causes illnesses affecting other organs, such as the brain, eyes and liver.
For example, more recent cases have developed neurological complications, including seizures, organ failure and stroke. It is estimated that about half of those infected with H5N1 will die.
The case of the Texas farm worker seems benign. This person had conjunctivitis, which is unusual.
Food safety
Contact with sick poultry is a key risk factor for human infection. Likewise, the Texas farmworker likely had close contact with the infected livestock.
The CDC says pasteurized milk and well-cooked eggs are safe. However, handling infected meat or eggs during cooking or drinking unpasteurized milk may pose a risk.
Although there is no H5N1 virus in Australian poultry or livestock, hygienic feeding practices are always a good idea, as raw milk or undercooked meat, eggs or poultry can be contaminated with microbes such as salmonella and E.coli.
If it’s not a pandemic, why are we worried?
Scientists have feared that bird flu could cause a pandemic since around 2005. Avian flu viruses do not spread easily among humans. But if an avian virus mutates to spread to humans, it can cause a pandemic.
One concern is that if the birds infected an animal like a pig, it would act as a vessel for genetic mixing. In areas where humans and livestock live in close proximity, such as farms, markets, or even homes with backyard poultry, the likelihood of bird and human flu strains mixing and mutating to cause a new pandemic strain is higher.
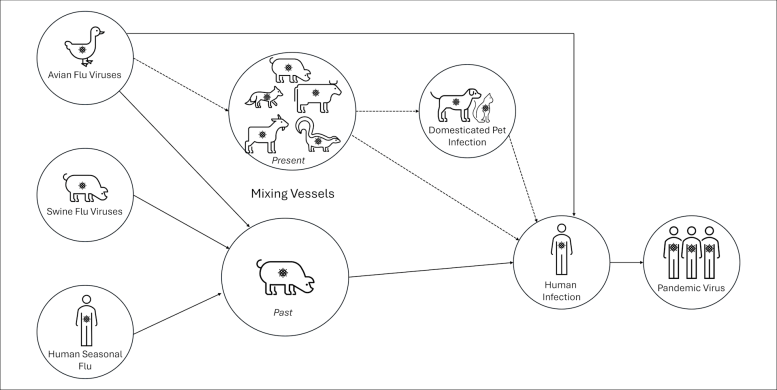
There are a number of potential pathways leading to an influenza-driven pandemic. Credit: Author provided
Infected cows in Texas were tested because farmers noticed they were producing less milk. If beef cattle are similarly affected, it may not be as easy to identify, and the economic loss to farmers could deter testing or reporting of infections.
How can we prevent a pandemic?
For the moment, there is no spread of H5N1 between humans, so there is no immediate risk of a pandemic.
However, we are now facing persistent and unprecedented infection with H5N1 clade 2.3.4.4b on farms, in wildlife, and in more wild birds than ever before, creating greater risks for H5N1 to mutate and cause a pandemic.
Unlike previous avian influenza epidemiology, where hot spots were in Asia, new hot spots (and likely sites for pandemic emergence) are in the Americas, Europe, or Africa.
Pandemics grow exponentially, which is why early warning of animal or human outbreaks is crucial. We may monitor infections using monitoring tools such as our EPIWATCH platform.
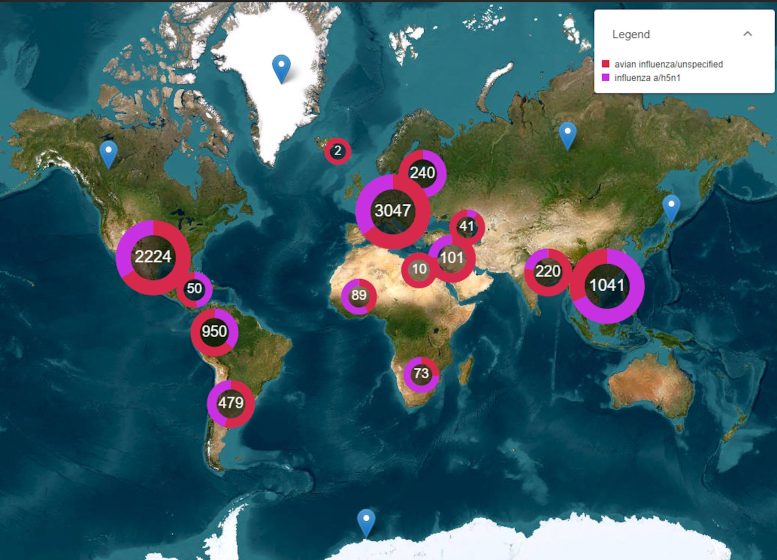
This map shows bird flu reports on EPIWATCH. Credit: EPIWATCH/author provided
The earlier outbreaks can be detected, the better the chances of eradicating them and quickly developing vaccines.
Although there is a vaccine for birds, it has been largely avoided until recently because it is only partially effective and can mask outbreaks. But it is no longer possible to control an epidemic by culling infected birds, which is why some countries such as France began vaccinating poultry in 2023.
For humans, seasonal flu vaccines can provide a small amount of cross-protection, but for optimal protection, vaccines must be exactly matched to the pandemic strain, and that takes time. The 2009 influenza pandemic began in May in Australia, but vaccines were available by September, after the pandemic peak.
To reduce the risk of a pandemic, we need to identify how H5N1 spreads to so many mammal species, what new pathways to wild birds pose a risk, and monitor early signs of outbreaks and disease in animals, birds and humans. Economic compensation for farmers is also crucial to ensure we detect any outbreaks and avoid compromising the food supply.
Written by:
- C Raina MacIntyre – Professor of Global Biosecurity, NHMRC L3 Researcher, Biosecurity Program Manager, Kirby Institute, UNSW Sydney
- Ashley Quigley – Senior Research Associate, Global Biosecurity, UNSW Sydney
- Haley Stone – PhD Student, Biosecurity Program, Kirby Institute, UNSW Sydney
- Matthew Scotch – Associate Dean for Research and Professor of Biomedical Informatics, College of Health Solutions, Arizona State University
- Rebecca Dawson – Research Associate, The Kirby Institute, UNSW Sydney
Adapted from an article originally published in The Conversation.![]()
News Source : scitechdaily.com
Gn Health